
Medicaid is a government-funded program that provides health insurance for the elderly and low-income. This program offers low-income people health insurance coverage, as well as funding for nursing home care. You or someone you love can request a fair Hearing if they have been denied Medicaid. Either you or an attorney can represent you at the hearing. It doesn't matter how you choose to represent yourself at the hearing, you will still need to submit a letter detailing your appeal. It must be submitted to the South Carolina Department of Health and Human Services no later than 10 days after your initial refusal. The state department will review your case and decide if you should continue to receive Medicaid benefits.
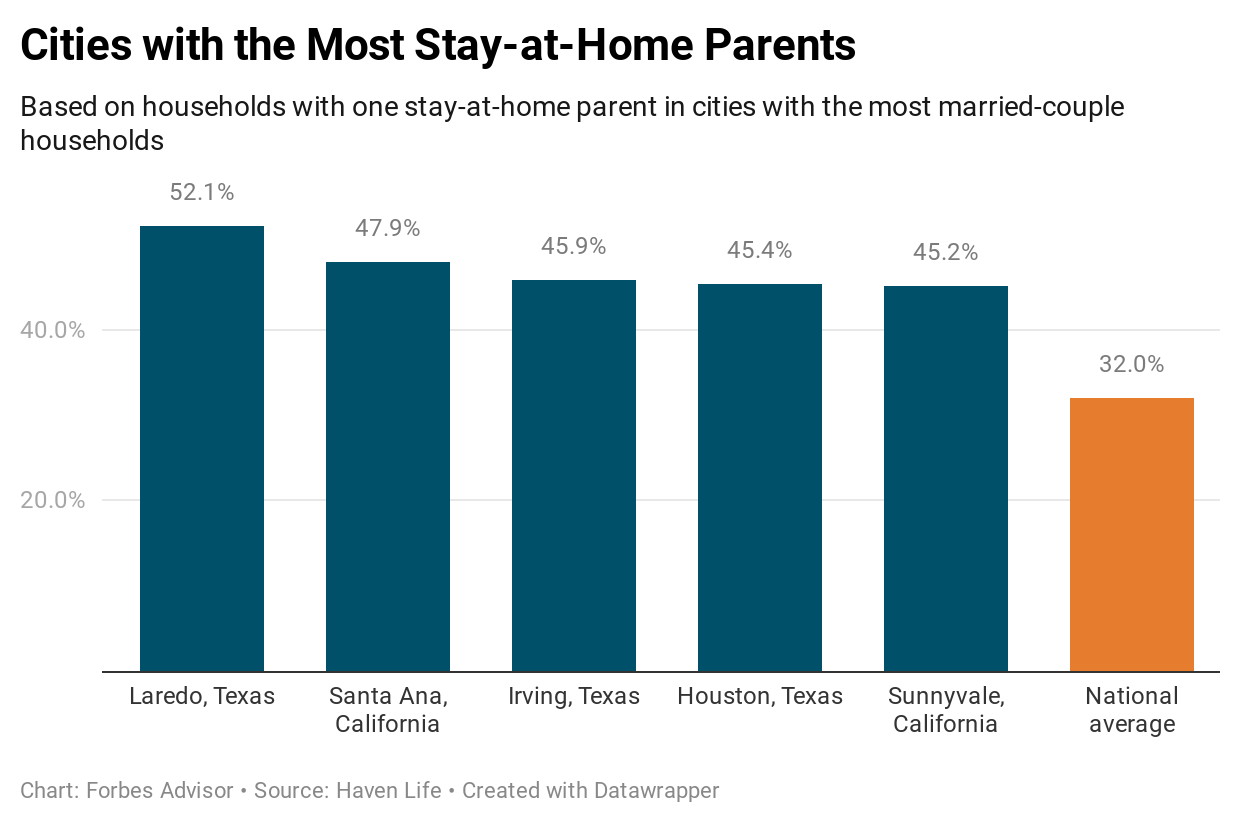
Medicaid is a government-funded health insurance program for the low-income, disabled and elderly
South Carolina Medicaid is an insurance program funded by the government that offers health insurance coverage to individuals, families, as well as seniors. Since 1965, the program's history is long and has seen significant expansion since its inception. It has also undergone changes as the Federal and State governments have worked to balance the many factors that affect its success. Medicaid, which was established in 1997, covered more than 33,000,000 people, making it the biggest health insurance program in America.
Medicaid is a government-funded health insurance plan that provides free health care to low-income residents. To qualify, applicants must reach 65 years or more and fulfill certain requirements. The program covers up to 10% of the costs of medication and doctor appointments and covers 90% of the cost.
It pays for nursing home care
Medicaid is a federal program to pay for nursing home services for eligible people. Medicaid pays for nursing homes in South Carolina via the Community Choices Waiver Program. This program allows residents to receive services in their own homes that are similar to nursing home care. These services include personal care, nursing, and therapy. In some cases, Medicaid will even pay for care provided by adult children of aged parents. These caregivers must pass background checks and can only be paid for their time.
Certain criteria are required to determine if you meet the eligibility requirements for Medicaid in South Carolina. You must meet certain income- and resource limitations to be eligible for Medicaid in South Carolina. The second is that you must reside in the state. You must also be at least 65 years of age and a citizen of the United States. Also, certain medical conditions must be met in order to receive the care you need. The care must be needed for at least 30 consecutive days.
You can be charged with fraud.
You may have heard about South Carolina's fraud penalties for Medicaid beneficiaries. Medicaid is concerned about fraud. The Medicaid Fraud Control Unit of the South Carolina State Attorney General's Office works in collaboration with auditors, investigators, and auditors to investigate fraudulent claims and prosecute them. This unit has experienced attorneys who are familiar with these types cases and have a solid understanding of the laws, procedures and regulations surrounding them.
Medicaid providers in South Carolina can be subject to administrative and criminal penalties for fraud. This law imposes strict penalties on Medicaid providers. It covers fraud in many ways, including the misrepresentation or abuse of financial data. Medicaid fraud penalties are also designed to ensure victims of fraud get full restitution.
It also offers an appeals process
If you've been denied Medicaid services by South Carolina, there are two options: to request a fair hearing or appeal. You can either represent yourself or hire a lawyer to represent you at the hearing. The appeals process begins by completing the request for a fair hearing form and submitting it to the Department of Health and Human Services. Upon receipt of the application, the hearing officer will review it and write a decision, which will be mailed to you. The decision will explain why you were denied service.
First, fill out the SCDHHSCR Form. An appeal can be filed within 30 days of the date the denial was made. The appeal will be rejected if the requested documentation was not received. This is why you need to submit your claim again.